Pancreatic tumor cells release large amounts of a protein called Tissue Factor into the bloodstream. This protein functions as the body’s primary “emergency trigger” for blood clotting, initiating the coagulation cascade—the complex sequence of reactions that ultimately forms a clot.
In addition, tumor cells shed microscopic particles containing Tissue Factor into circulation. These particles travel throughout the bloodstream, spreading clot-promoting signals to distant areas of the body. They frequently lodge in the legs, where clot formation often occurs.
Adenocarcinoma Mucins
Another important contributor involves mucins—large, sugar-coated proteins produced by many pancreatic tumors. When these mucins enter the bloodstream, they behave like adhesive bridges, attaching to platelets and white blood cells. This interaction activates them in ways that strongly encourage clot formation.
Together, these mechanisms create what physicians sometimes refer to as “sticky blood”—a condition in which the body’s natural clotting system remains continuously activated, making it far more likely for dangerous blockages to form.
Why the Legs Are Affected
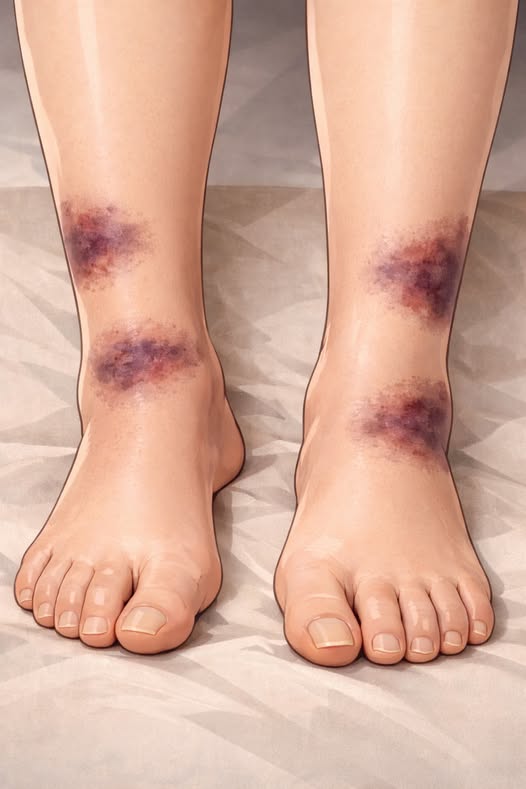
According to research published in the National Library of Medicine, blood naturally moves more slowly through the deep veins of the legs than in many other parts of the body. This happens because gravity works against the upward flow of blood and because the legs are located far from the heart. As a result, this region is particularly vulnerable to the development of blood clots.
When abnormal clotting signals circulate throughout the body, the legs are one of the most frequent locations where a blockage can develop. As a clot begins to form, it disrupts normal blood flow and quickly leads to swelling and inflammation in the affected area. Some individuals may also notice pain, warmth, or redness, but for many patients the only visible warning sign is swelling in the leg.
Recent Articles

The ring you choose reflects your personality.

Pecan Cream Pie

Cases are on the rise